Introduction
The first line of treatment of erectile dysfunction (ED) is currently shifting from specialty care and
subspecialty care to primary care offices. This shift is primarily due to the availability of the new
oral medication Viagra®
(sildenafil citrate). The following is an overview of how Erectile dysfunction can be treated safely
and effectively in the primary care setting.
Historical Perspective
From Psych to Medicine: Prior to the early 1980's erectile dysfunction was thought to be mostly a psychological problem. Advances in the understanding of erectile physiology combined with new epidemiological research have caused a major paradigm shift in the clinical concept of erectile dysfunction. What had been called a psychological problem came to be seen as more of a physical problem. This change resulted in the increased use of vacuum erection devices and penile prostheses, and effective medical and surgical treatments that had existed since the late 1960s. These treatments had been in use since the early 1970s and before, but had been underutilized in favor of counseling approaches.
The next phase of treatment evolution was the initiation of intercorporal injection therapy with papaverine, and then prostaglandin in the mid-1980s. This form of treatment gained popularity because it gave a more "natural" feeling of erection than a vacuum device or prosthesis did, required no surgery, and could be put to use when needed with relative ease. Prostaglandin (to maintain a patent
ductus arteriosis in neonates) and papaverine (for hypertension) were in use in "off label" ways for 10 years and were available almost exclusively from the local urological offices that would repackage
and sell them. The release of Caverject
® (alprostadil injection) by the Upjohn Company in September 1995 made effective treatment for erectile dysfunction available in the local pharmacy for the first time. The release
of MUSE® (alprostadil), a urethral prostaglandin suppository, in January 1997 represented an attempt to make intracorporal injection medication available for use without a syringe, thus increasing its acceptability to the general public.
Erectile physiology and pathophysiology
The following has been accepted as a paradigm of erection only since around 1980. All currently available treatments effect the corpora cavernosa. They do not do anything to the glans and none of these treatments directly effect the rigidity of the glans (head of the) penis.
Gross anatomy of the penis
The penis is mainly made up of the corpora cavernosa. The corporal bodies are two cylinders that start back separately on each of the pubic rami and then come together and form the dorsum of the
penis, ending right behind the glans of the penis. The other main chamber of the penis is the corpora spongiosum, which surrounds the urethra on the bottom and then flares out to form the glans of the penis at the tip.
Both these structures are flimsy, spongy tissue which can fill with blood. What makes the cavernosal bodies rigid when they become blood-filled is the tough membranous sheath around them called the tunica albuginea. The filling sponges of the corporal bodies press against this relatively inelastic membrane and thus cause increased intrapenile pressure and rigidity.
Neurological aspects of erection
Erections start with a neurological signal, sort of like turning the ignition of an automobile sends a spark to the spark plugs. The parasympathetic and sympathetic neurological pathways leading to the penis and the sensory pathways are the same ones that are involved in voiding. The sympathetics are from spinal level C10 to L2. Sympathetic innervation is generally considered to control ejaculation and detumescence (i.e. "deflation" of the rigid penis). The parasympathetics innervating the penis are from spinal level S2 to S4. These parasympathetics lead to the cavernosal nerve, which will deliver the "spark" to start an erection. The parasympathetics also lead away from afferent fibers of the dorsal nerve of the penis, signaling the sensation of physical contact with the penis.
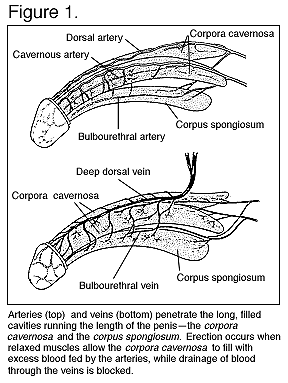
Vascular aspects of erection
The main blood supply to the corporal bodies of the penis is the cavernosal artery. The curlique-shaped helicine arterioles branch off from the cavernosal artery and sends arterial blood to the trabeculae that surround it. This trabecula in the cavernosal bodies has in it
the vascular bed that is the target organ of neural initiation of erection. It is made up of smooth muscle and structural elements that surround the spaces in this vascular bed where blood flows in and out of the penis. These spaces are called lacunar spaces (or sinusoids). The size of these spaces, and thus the volume of blood they can hold, is determined by how contracted or relaxed the smooth muscle in the trabeculae are that surround them. When the penis is flaccid (soft) the smooth muscle is contracted (tight). When the penis is rigid, the smooth muscle is relaxed. Relaxed smooth muscle gives the vascular space more room to stretch, and therefore fills up.
Arterial inflow to the penis occurs relatively deep to the membranous sheath called the tunica albuginea that surrounds the corporal bodies. This sheath acts to restrain the expansion of the
corporal bodies of the penis as they fill, thus causing increased intracorporal pressure and increased penile rigidity. Venous outflow occurs through a system of venules and veins that are relatively more superficial than arterial inflow. When intracorporal pressure increases, these venules and veins get squeezed closed by the increasing pressure. At maximal rigidity there is actually no inflow or outflow of blood, but in most men that situation does not last very long.
This vascular system of relatively deep arterial inflow and relatively superficial venous outflow explains why you can constrict the penis with some type of ring and only restrict venous outflow. Since
incompetency of this veno-occlusive mechanism of the penis is the most common cause of erectile dysfunction of a vascular nature, many men may benefit to some degree from using a constriction device. An example of a commercially available product is the
Actis® venous flow controller.
It is both possible and in many instances preferable to treat men for erectile dysfunction in the primary care setting. To do so you need to understand erectile physiology, understand the treatment options, be able to evaluate men's complaints in this area, and be sensitive to the fact that treating erectile dysfunction is not always the same as treating sexual dysfunction. The following is a discussion of the clinical evaluation of men with erectile dysfunction.
A Model of Male Sexual Activity
male sexual activity = libido (desire) + ability + opportunity This model is perhaps simplistic, but its practical aspects make it very applicable to the primary care setting. For example, the model predicts that a man who can no longer get erections but has a healthy libido, is in a sexual relationship, and can engage in sexual activities that do not require a rigid penis will not necessarily be attending clinic for treatment of his ED. It also predicts that men with ED who come for treatment but are not in a sexual relationship will have a hard time evaluating whether treatment has been successful.
Men self-identified as having ED may or may not have ED. This is because men are not generally in the habit of discussing sexual functioning in a clear, precise way. What men describe at first as erectile dysfunction may on further questioning be a totally different problem. Therefore, when men come in to clinic seeking treatment, your first task will be to determine whether they are there for ED treatment or whether they have some other type of sexual dysfunction. This is a short list of sexual dysfunctions in men:
- Excitement – decreased/absent libido
- Attaining erection – ED; painful erection; chronic/acute pain
- Maintaining erection – premature/rapid ejaculation; delayed
- Orgasm – anorgasmia; painful ejaculation
- Ejaculation – anejaculation
A man whose primary problem is really depression, or perhaps even the lack of a sexual partner, may present as having decreased libido until you clarify the situation. A man may state he has ED but may instead be experiencing pain with erections (most commonly caused by Peyronie's Disease) which may make him not want to get erections. Conditions causing chronic or acute pain may effect many activities including sexual functioning, causing some men with normal erectile capability to tell you that they have ED. Men whose only problem is that they do not maintain erections long enough (premature ejaculation), or have delayed ejaculation may also initially tell you they have ED. Finally, men with difficulties attaining orgasm or ejaculation may state they have ED (many men will also use the words ejaculation and orgasm synonymously).
In short, the treatment of erectile dysfunction in primary care will first require confirmation that the problem is indeed erectile dysfunction and not something else. After full evaluation will come treatment. The goal of treatment of ED in primary care is to assist the patient in self-selection of a method of treatment. The treatment of ED is in that way kind of unique. Your goals will be to maximize the chances of success, minimize the adverse affects of treatment, and then to appropriately refer to specialty care when needed. All this has become much easier to do in primary care with the release in April 1998 of the new oral medication Viagra® (sildenafil citrate).
Approach to the Clinical Care of the Man with ED
A couple years ago all there was to offer in treating erectile dysfunction in primary care was intracorporal injections and vacuum erection devices. Those treatments did not excite a lot of interest from primary care providers because they can be hard to work into primary care practice. Assuming a man has no contraindications for its use, the institution of ED treatment with sildenafil (Viagra® or sildenafil citrate) is relatively simple. And while this treatment may not work for everyone, trying treatment once may encourage patients to try other treatments until a successful one is found.
How is this started? Beginning with finding out what kind of sexual dysfunction the patient has. If indeed they have erectile dysfunction you may then move on to appropriate treatment.
The first step is to find out about what kind of problems the patient is having with their penis. The "PLISSIT" model of initiation of sexual therapy is a guide to the process of evaluating men for treatment of erectile dysfunction. It stands for:
"P"ermission
"L"imited
"I"nformation
"S"pecific
"S"ugestions
"I"ntensive
"T"reatment
The last line really refers to sex therapy which generally occurs outside of the primary care setting and will not be addressed here. Asking permission means making sure the patient feels comfortable with talking about the subject of sexual functioning before continuing. You can generally start out by simply asking "How can I help you today?". Most men will start telling you about the problems they are having with erections right off. But the men who start talking about parking, or traffic, or
extensively explain their medical history will need more time and more psychological space before they are going to feel comfortable talking about why they are there.
The next phase of the "PLISSIT" model is limited information. After gaining permission to discuss ED it is a good idea to spark the patient's interest in the topic, and also try not to overwhelm them. This might be done by stating something neutral like "there are treatments available nowadays for erection problems that many men are using" and see what the response is. If the response is a positive one, the provider can proceed to the next part of the model by offering specific suggestions, i.e. a prescription and a plan of care. Sex therapy is a very helpful adjunct to the care of many men with ED, but I also find that it is very difficult to get them to go to it generally because of reimbursement and time issues.
Practical Aspects of Clinical Evaluation
Most primary care providers are going to see the established patients with ED, because those men will be the most comfortable seeing someone about this problem. Clinical care of the man with ED will start with a history. Know how long the problem has been going on, any chronic illnesses or possible causes of ED, prior treatments for ED and then whether or not the patient's libido (i.e. interest in sex) is intact. You will also want to know about their relationships or social situations, which can be the best predictor of successful treatment overall. In general men in a stable sexual relationship have the greatest success with any treatment. In a stable relationship, communication is better and couples tend to work problems out. Men who are not in stable relationships, who hope to be made super-normal are going to be more difficult to treat. Men who are single or in less secure relationships also frequently request treatments that lend themselves to spontaneity of sexual expression, which none of the non-surgical
treatments currently do.
A good history will give some idea of what men can expect, so when men call and say that they are having problems with treatments not working, the history can give some idea of how to interpret what they mean by "not working". Is the patient somebody who has been married for 20 years and has a stable relationship, or is it somebody who has not been able to find anybody to date and that is why it is not working?.
Taking a history begins with knowing if the patient is a new or a return patient. The reason for this is that the more you know this patient and the more in-depth information you have about their medical problems, the better you will be able to formulate reasons why they are having erection problems. A patient who is 25 or 30 years old who comes in with erectile dysfunction, comes in as a new patient, and who does not have any other obvious medical problems that they know about, may take more time to evaluate and may require a complete physical.
The next thing you want to know is how long this problem has been going on. Men who tell you they've had ED for 20 years and are now first seeking treatment will be different to treat than those who say I have recently had a prostatectomy and now I want to see if Viagra® (sildenafil citrate) can help me.
It is important to know if the patient is having any pain with erection and any bending, shortening or narrowing of the penis. This will help confirm what kind of sexual dysfunction they have, i.e., someone may have Peyronie's disease, get a pretty rigid erection still but it hurts and it bends severely.
Also know about the patient's libido, or whether they are interested in sex. Most of the men are going to have a normal libido or else they may not even care if they are having good erections or not. Other men may be seeking treatment for ED because their long term partner has suggested that they go do so. For men whose libido is lower, especially men who are over 60 yearsof age, it might be worth checking their testosterone levels. If low, replacement may be made with exogenous testosterone. A provider should expect such replacement to increase libido only. Testosterone replacement will have little if any direct effect on erections, other than giving the patient the desire to get them. If testosterone replacement is being considered, a complete prostate cancer screening (i.e. rectal exam and serum PSA measurement) should be done since testosterone is a promoter of prostate cancer (Testosterone is not a cause of prostate cancer, more of a fertilizer for it).
Knowing about the last time the patient attempted sexual activity sets the stage for how successful these treatments may be. Someone who has not attempted any type of sexual activity for a very long time will have more difficulty instituting a successful treatment for erectile dysfunction than someone who engages in sexual communication with their spouse or partner at regular intervals.
Know whether or not the functions of ejaculation and orgasm are intact. If a patient calls and says treatment is not working it is important to know if what they really mean is that their erections are much firmer but that they are not ejaculating or not having orgasm.
The physical examination you perform is the choice of the provider. Consider prostate cancer screening if testosterone replacement is being considered. Examine the penis if there is pain or bending reported. Briefly stated, the penis can be examined by first grabbing the glans in a pincher grip of the thumb and forefinger. Then use the other hand to palpate the dorsum of the penis from base to tip using a kind of an upward pincher with the thumb and forefinger of the dominant hand, sort of rolling the upper part of the corporal bodies between the fingers. The dorsal junction of the two corporal bodies is the
most common place to find plaques or thickening from collagen. After palpating the dorsum, repeat the procedure on the ventral side, again from base to tip. It is not a difficult maneuver to do, but it takes a lot of practice to know what is being felt. As a provider, don't be frustrated if you find this procedure difficult, and don't worry about how to document on paper exactly what you find, as both are hard to do, even for the experts.
Also important to note is if you do a genital or rectal exam, also do a scrotal exam. The yield is going to be very low but this is more a medical legal consideration. If somebody has been in clinic, been examined, but a scrotal exam has been neglected, and later on they develop or find that they have testicular cancer, the provider may be embarrassed and may even go to court.
Treatment
If the patient has considerable pain or bending of their erections, consider a referral. If they have low libido, a testosterone level may be needed. If there are other problems present, expect poor treatment results and consider a referral.
The current first line treatment for erectile dysfunction in both primary and specialty care is oral sildenafil citrate (Viagra®). As described later on, it is relatively easy to use and relatively safe. If the patient can not use sildenafil citrate (Viagra®) they should be referred or offered another treatment if that is something available at the practice. It is also possible that the patient may not be interested in any treatment available. If not, they should be asked to return if they ever change their mind.
Jeremy Heaton in 1997 came up with a paradigm, illustrated below, to categorize current and potential medical treatments for erectile dysfunction. He categorized things as to whether they act centrally or peripherally, and whether they initiate (start) or condition (facilitate) erections. In this paradigm sildenafil citrate (Viagra®) is a peripheral conditioner, in other words it amplifies the corporal tissues' response to the neurological signal to initiate an erection. On the other hand, intracorporal (penile) injections are a peripheral initiator, in that they provide the spark that starts an erection by directly supplying nitric oxide to the tissue. A drug in development by TAP Pharmaceuticals is a sublingual form of apomorphine. This drug will be a central initiator, increasing the intensity of appropriate neurological impulses down to the penis to cause erection.
|
Central Action |
Peripheral Action |
| Initiate |
apomorphine1 |
intracorporal injections
Caverject®
MUSE®
|
| Condition |
|
Viagra® |
| Other |
constriction rings
vacuum erection device |
1. In development by TAP Pharmaceuticals
How does sildenafil citrate (Viagra®) "condition" an erection in response to stimulus? Current thinking is that nitric oxide is the spark or initiator that causes relaxation of the smooth muscle in the little lacunar spaces of the corporal tissues. Nitric oxide causes cyclic GMP to be formed in the corporal smooth muscle, which causes an efflux or outflow of calcium from those smooth muscles, thus causing relaxation. Sildenafil citrate
(Viagra®) does not initiate the erection in that it does not bring a source of nitric oxide into the penis. Sildenafil citrate (Viagra®) works by inhibiting the degradation of cyclic GMP, by slowing the rate at which the body gets rid of it. It does this by inhibiting the phosphodiesterase enzyme mostly responsible for disposing of nitric oxide in the penis, namely PDE-5.
Nitroglycerin is a superb nitric oxide donor. If a patient were to take a nitroglycerin tablet and a sildenafil citrate (Viagra®) together, the sildenafil citrate
(Viagra®) will inhibit the degradation of that nitric oxide from the nitroglycerin. That will in effect greatly multiply the amount of nitric oxide donated by a single dose of nitroglycerine-type medication.
The most important thing to tell patients about sildenafil citrate (Viagra®) is not to use it if they use nitrate-type medication. One should not prescribe sildenafil citrate (Viagra®) for anybody who is on any form of nitrate, which at times makes for difficult clinical situations. One way to handle that is by counseling patients on how to use sildenafil citrate (Viagra®) should they get a prescription. Then tell them that the provider who prescribes nitrates for them needs to be the one to prescribe sildenafil citrate
(Viagra®). Also tell them that the expectation will be that the prescriber will reassess their need for nitrates, and if nitrates can be completely dropped from their medication regimen then it is safe to use sildenafil citrate (Viagra®). For example, men who take nitrates for gastroesophageal reflux may be able to control that problem without nitrates.
Another treatment for erectile dysfunction well suited for primary care prescribing is the vacuum erection device (VCD). Nobody really understands how they work, but it is generally reported that the reason they work is that they occlude the venous return from the penis. Medicare reimburses 80% of the allowable charge for them, and they are effective for many men. However, not all men like using them either because they think they are mechanical or they dislike the way the constriction rings feel. For many men who use them the rings themselves cause retrograde ejaculation by blocking the urethra.
A urethral suppository of prostaglandin (an initiator, or nitric oxide donor) called MUSE® (alprostadil) has been on the market since January 1997. As mentioned earlier, the urethra is surrounded by the corpora spongiosum. Once placed in the urethra, the medication is supposed to absorb into the spongiosum and then travel to the corpora cavernosum. It does this through a backflow in the venous drainage system of the penis. I find this medicine works in fewer than 20% of the men I try it with. Given that the most common cause of vascular-based impotency in the U.S. is the failure of the venal occlusive mechanisms in the penis, it is not suprising that this absorption method through the venous return system does not work well for many men.
Constriction rings are inexpensive and can be either a primary or adjunct (used with another) treatment. Some men do not like using them, other men it does not seem to bother. If somebody is using sildenafil citrate (Viagra®), and it is almost good enough, they can go purchase and try a constriction ring with it.
Intracorporal injection is often the most reliable form of treatment that is available. It works in about 65% of the men it is tried with, and it is an initiator of erection because it is a direct nitric oxide donor to the corporal tissue. Treatment is applied by injection medication with an insulin syringe directly into the corpora cavernosa on one side. Many men dislike doing this type of injection, which is one of the major problems with this form of treatment. With the release of sildenafil citrate (Viagra®) many men who were previously thought to be very happy on injection therapy said they would really like to get rid of the needle if possible. Injection therapy can cause abnormal depositions of collagen in the penis, causing bending, shortening, or narrowing of the penis. It can also on occasion cause prolonged erections (erections that last for four hours or more that need medical attention to help become non-rigid again), but proper instruction in usage helps control the incidence of that side effect.
Finally comes follow-up. Did the patient attempt sexual activity at any time? Did he try the treatment when he did? Did he use it as prescribed? Did the treatment work, by whatever their definition of "worked" is (ask the patient to define it). Ask about problems, side effects, and number and types of attempts. If treatment is working, use discretion regarding future follow-up. If it is not, either consider a constriction ring with the primary treatment or making a referral to specialty care. It is also quite possible that your patient will say, "For now, I'm not interested until the next treatment comes along." And there are a lot of new treatments coming along.
Resources
Handouts and Educational Information
What Patients May Be Reading
Updated May 9, 2000
Use of this section indicates you agree to the Terms of Use.
Copyright 1994-2003 NP Central
| 






